Immunomodulatory Role of Mesenchymal Stem Cell Therapy in Multiple Sclerosis: A Systematic Review
Abstract
The progressive immune-mediated disease known as multiple sclerosis (MS) is characterized by myelin degradation, inflammation, and neurodegeneration. Recent research has examined the potential of mesenchymal stem cell (MSC) therapy for treatment, focusing on its neuroprotective and immunomodulatory properties. This study looked at how MSC transplantation affects cerebrospinal fluid (CSF) biomarkers and the immune system, and checked whether they can indicate the safety and effectiveness of the treatment for MS. According to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines, this systematic review was conducted. The final selection comprised eight studies: two randomized controlled trials (RCTs), two non-randomized experimental studies, three systematic reviews with meta-analyses, and one narrative review.
Following MSC therapy in MS patients, significant alterations in neuroprotective biomarker levels were found in the CSF, exhibiting positive results. Immunologically, MSC therapy facilitated the expansion of regulatory T cells (Tregs) and suppressed T helper type 17 (Th17) cell activity, restoring immune balance and diminishing neuroinflammation. Clinically, improvements in Expanded Disability Status Scale (EDSS) scores and MRI lesion burden were observed in a significant subset of patients. Across the included studies, MSC therapy was generally safe, with mild, self-limiting adverse effects. However, heterogeneity in MSC sources, administration routes, and outcome measures, along with small sample sizes, limited comparability. In conclusion, MSC-based therapies show promising potential as a personalized approach to MS management.
Introduction & Background
Multiple sclerosis (MS) represents an inflammatory, immune-mediated disorder of the central nervous system (CNS), characterized by multifocal demyelination and subsequent neuronal degeneration [1]. MS represents the predominant non-traumatic etiology of disability among young adults, affecting more than 2.8 million individuals worldwide and exhibiting a notable rise in incidence in recent decades [1]. Earlier research has demonstrated that immune dysregulation in MS primarily stems from myelin-specific autoreactive CD4+ T cells and is strongly linked to immune dysfunction, temporary activation of immune cells, and an imbalance in immune cell subpopulation ratios [2,3].
Upon activation, naive CD4+ T cells undergo differentiation into T helper type 1 (Th1) and T helper type 2 (Th2) helper subsets, as well as T helper type 17 (Th17) cells and regulatory T (Treg) cells. Significantly, the heightened pro-inflammatory effects of Th17 cells, along with the reduced immunosuppressive ability of Tregs, are essential elements contributing to the breakdown of immune tolerance in MS [4].
Despite notable progress in recent decades, a proven cure remains elusive, and the available treatments have drawbacks that prevent their use in clinical settings due to undesirable side effects [5,6]. At present, there are numerous immunotherapies available, aimed at restoring the balance of Th17/Treg in MS. These include a range of disease-modifying therapies (DMTs), immunosuppressive agents such as interferon beta (IFN-β) [7], glatiramer acetate (GA) [8], teriflunomide, and fingolimod, in addition to several monoclonal antibodies that employ cell depletion strategies [9].
In MS patients, the Th17/Treg imbalance has been somewhat alleviated by these DMTs and other monoclonal antibodies based on cell depletion therapy [10]. However, with a higher risk of infection, tumors, and other negative effects, these medication therapies are nonspecific and suppress the systemic immune system [10,11].
The primary objectives of most currently available therapeutic approaches, which are based on the prescription of immunosuppressive and immune-modulating treatments, are to reduce symptoms, reduce the rate at which disability develops, avoid relapses, and limit disability accumulation [5,6]. Recent studies have shown that mesenchymal stem cells (MSCs) possess strong immunomodulatory potential [12], which makes them extremely promising options for the management of inflammatory autoimmune diseases [13].
MSCs possess significant immunomodulatory properties and exhibit low immunogenicity; they are regarded as a crucial resource for managing the progression of MS and re-establishing immune tolerance. In addition, a deeper understanding of the possible mechanisms behind MSC-mediated Th17/Treg homeostasis is necessary to support the creation of novel MSC-based treatments, targeted at more accurate immune-molecular interventions, and to increase the viability of using MSCs as a type of cell therapy in the clinical treatment of MS [14].
MSCs substantially enhance both innate and adaptive immune responses due to their anti-inflammatory, anti-apoptotic, and immunomodulatory qualities. The immunomodulatory effects may result from direct interactions with immune cells or through the paracrine signaling mechanisms of MSCs [15,16]. These cells belong to a class of non-hematopoietic stem cells (HSCs), distinguished by their ability to self-renew. Since their initial extraction from bone marrow, these cells have been found in several other tissues, including the periendothelium, adipose tissue, epidermis, and umbilical cord blood [17]. They possess a remarkable ability to differentiate into cells representative of diverse mesenchymal lineages, including osteoblasts, chondrocytes, fibroblasts, and adipocytes, when exposed to suitable stimuli [17].
MSCs can display diverse surface markers and cytokine profiles, influenced by their tissue of origin [18]. They play a crucial role in preserving immunological and vascular balance, as well as assisting the bone marrow’s HSCs. This is achieved through their capacity to migrate selectively to areas of tissue injury or inflammation – a process known as “homing.” MSCs have been the subject of extensive research across various disease models due to their accessibility as a source of either autologous or allogeneic somatic stem cells, which possess the potential to differentiate into multiple cell types [19]. Consequently, novel treatments such as MSC therapy have demonstrated encouraging outcomes in addressing severe MS. By repairing injured nerve cells and halting the progression of the disease, these advanced therapies provide renewed hope for patients who have not adequately responded to traditional treatment methods [6]. Recent RCTs have demonstrated the neuroprotective and immunomodulatory effects of MSC therapy – particularly its impact on cerebrospinal fluid (CSF) biomarkers – which, in turn, influence the progression of the disease [20,21].
Although MSCs are known to modulate immune responses, their exact mechanisms, particularly in regulating the Th17/Treg axis in MS, remain unclear. Addressing these gaps is essential for advancing targeted therapies and improving clinical outcomes. Moreover, several unanswered questions regarding their mechanistic role highlight the need for further research. Therefore, this systematic review aims to synthesize clinical evidence on the immunomodulatory and restorative effects of MSC therapy in MS, with a focus on inflammatory markers, immune balance, and clinical endpoints. This review seeks to clarify the therapeutic potential of MSCs and identify key areas for future investigation.
Review
Methods
To create this systematic review, we precisely followed the 2020 guidelines for the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) [22].
Eligibility Criteria
We chose the studies according to the elements of Participants, Intervention, and Outcomes (PIO): Participants – MS patients; Intervention – stem cells, MSCs; and Outcome – immune response, an immunomodulatory outcome measure. Furthermore, we implemented additional inclusion and exclusion criteria. The inclusion criteria encompassed English-language full-text articles disseminated within the preceding five years, as well as RCTs, systematic reviews, observational studies, meta-analyses, and reviews. The exclusion criteria comprised case reports, case studies, and editorials.
Selection Process
We imported all relevant articles into EndNote (Clarivate, Philadelphia, PA, USA) and grouped and alphabetized all references using Microsoft Excel 2021 (Microsoft® Corp., Redmond, WA, USA) for duplicate removal. Each identified article underwent a preliminary screening process that involved examining titles and abstracts. Following the identification of eligible articles, we evaluated the availability of their full texts. The most pertinent papers were assessed based on predetermined inclusion and exclusion criteria. We included articles that met all specified criteria in the study. Conversely, we excluded studies that did not provide the necessary analyses for this review. Any disagreements between the reviewers during the study selection or quality assessment phases were initially resolved through discussion; if consensus could not be reached, a third independent reviewer was consulted to reach a final decision. The researchers opted to include systematic reviews, meta-analyses, and narrative reviews in the study, due to the limited number of such works in the field.
Databases and Search Strategy
We systematically searched PubMed, PubMed Central (PMC), Cochrane Library, Google Scholar, and ClinicalTrials.gov for relevant studies published up to March 24, 2025. The search strategy included combinations of Medical Subject Headings (MeSH) and free-text keywords related to “Multiple Sclerosis,” “Mesenchymal Stem Cells,” “Immunomodulation,” and related terms. Boolean operators and database-specific filters (e.g., full text, English language, and last five years) were applied. The complete search strategy is detailed in Table 1.
Risk of Bias in Individual Studies
We evaluated the remaining full articles for quality and bias risk using specific tools tailored to the type of study by extracting relevant data using a predefined template and implementing commonly employed evaluation tools for each study. We utilized the Cochrane Collaboration Risk of Bias Tool (CCRBT) for RCTs; we employed the Joanna Briggs Institute (JBI) Critical Appraisal Checklist for quasi-experimental studies; we used the Assessment of Multiple Systematic Reviews 2 (AMSTAR 2) for systematic reviews and meta-analyses; and we used the Scale for the Assessment of Narrative Review Articles 2 (SANRA 2) for narrative reviews [23-26]. Each of these assessment tools had distinct criteria and scoring systems. A score of one point was awarded for ratings of “LOW RISK,” “YES,” “PARTIAL YES,” or “1,” while two points were assigned for a score of “2.” A minimum score of 70% was required for acceptance from each assessment tool (Table 2). A >70% threshold was selected to ensure inclusion of studies with acceptable methodological quality, consistent with practices in prior systematic reviews.
Data Collection, Items, and Analysis
This systematic review describes these trials and reviews based on their outcomes, applicability, and limitations, using a narrative synthesis rather than performing a meta-analysis because of the inter-variability among studies, including the heterogeneity of participants, the variety of interventions, and the range of outcome measures. Full articles were read, examined, and tallied for reviews and clinical trials. First author, year, study type, disease, inclusion and exclusion criteria, results, key findings, and funding sources were among the items collected from each study. We added the sample size and demographics of research participants for clinical trials. The reviews addressed the total number of participants and the variety, quantity, and type of studies.
Results
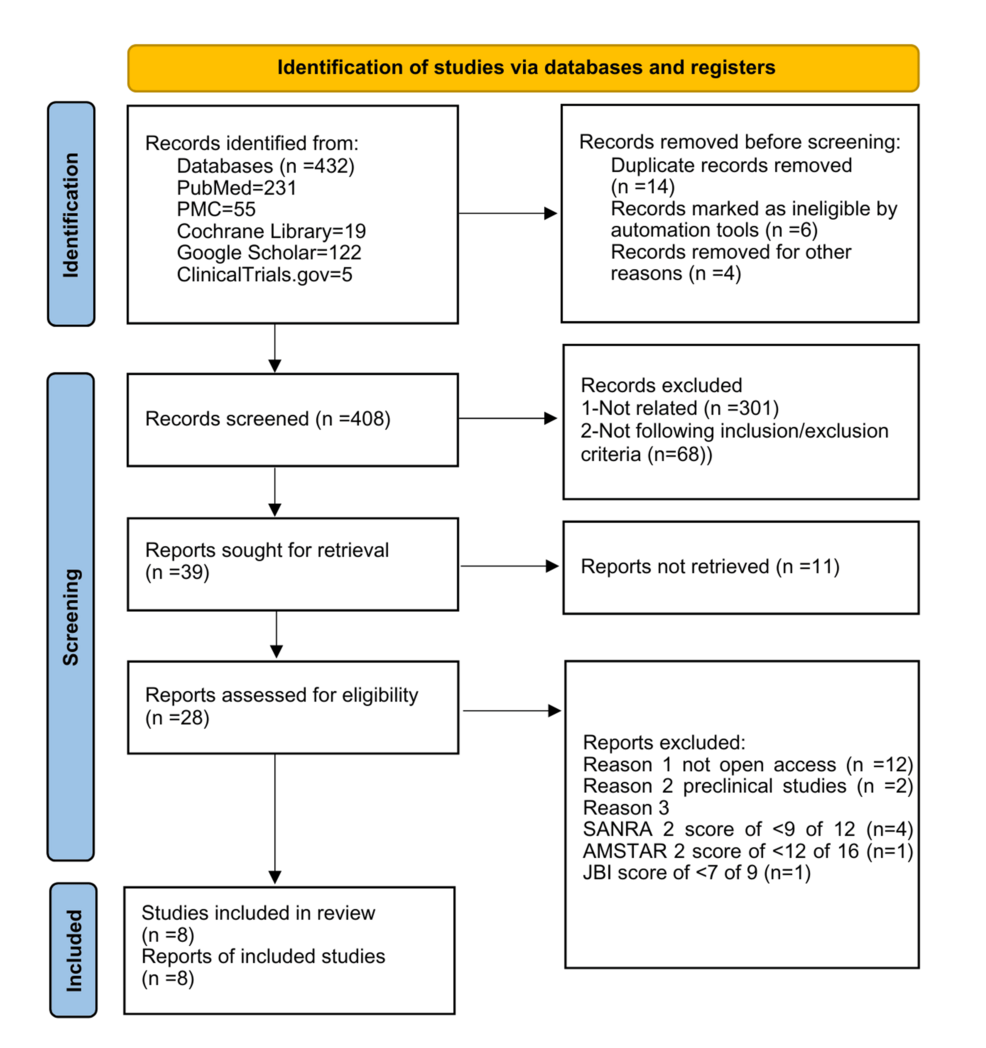
The initial number of relevant studies identified on PubMed, PubMed Central, Cochrane Library, Google Scholar, and ClinicalTrials.gov was 432. EndNote, in total, removed 14 duplicated articles, removed six records by automated tools, and removed four for other reasons. We performed an extensive review of 408 articles, which included a thorough examination of titles and abstracts, as well as an evaluation of full-text accessibility. As a result, 39 articles were chosen for retrieval, while 369 were eliminated from further consideration. After further assessment of the chosen studies, it was determined that 11 reports were not retrievable. Ultimately, we assessed 28 pertinent articles for eligibility and quality based on established appraisal criteria.
Accordingly, we excluded six studies with scores lower than 70%, 12 studies not open access, and two preclinical studies. As a result, we incorporated eight pertinent articles into the systematic review. Articles with favorable and unfavorable outcomes were selected to mitigate the risk of bias. Figure 1 illustrates the PRISMA flowchart depicting the selection and screening methodology.
The following tables show how each study was evaluated using the corresponding quality assessment tool for each type of study. All RCTs assessed in the review, used the CCRBT and exhibited a “LOW RISK” of bias concerning generating random sequences.
The JBI Critical Appraisal Checklist for quasi-experimental studies (non-randomized experimental studies) was used to assess two quasi-experimental studies in the review [24]. Item 4 was recorded as “NO” for those two studies because there was no control or comparator (Table 3).
In order to assess the possibility of bias in RCTs, the Cochrane Risk of Bias 2 (RoB 2) Tool Scoring was applied to these studies, as shown in Table 4. Selection, performance, attrition, reporting, and other domains were among the five areas where bias was measured as a judgment (high, low, or ambiguous) for certain elements.
Three studies were systematic reviews with meta-analysis. Upon scoring using the AMSTAR 2 tool, all accepted reviews had “NO” in Item 10. One review had “NO” in Item 7. These discussed funding sources and heterogeneity, respectively, as presented in Table 5.
Finally, Table 6 illustrates the evaluation of narrative reviews utilizing the SANRA 2 checklist, which comprises six criteria. The accepted review received a score of “1” for its literature search description and the suitable presentation of data.
Study Characteristics
The following tables show, chronologically, the main characteristics of clinical trial studies (RCT and non-RCTs) and reviews (systematic reviews, meta-analyses, and narrative reviews). Of the eight studies accepted in the review, three articles focused on a population of progressive MS patients (Secondary progressive multiple sclerosis (SPMS) and primary progressive multiple sclerosis (PPMS)), while five studies examined all MS patients (including relapsing-remitting multiple sclerosis (RRMS), SPMS, and PPMS).
There were 157 participants with MS in the RCTs and non-RCTs. Forty-eight patients received MSC transplantation, either intrathecal (IT) or intravenous (IV); 20 participants (two dropouts) received three IT administrations of autologous mesenchymal stem cell neurotrophic factor (MSC-NTF) cells; 54 participants (seven dropouts) received six IT injections of autologous mesenchymal stem cell-neural progenitors (MSC-NPs). A total of 35 participants received two treatment protocols involving the administration of umbilical cord-derived mesenchymal stem cells (UC-MSCs) via IT and IV routes. The study lacked a control group and was designed as a non-RCT with an open-label format. Table 7 shows these findings.
There were 9, 18 RCTs, 30 studies in systematic review, 22 studies in meta-analysis, and various clinical trials (phase I/II, pilot studies without exact number) in the four reviews, respectively. These reviews provided explicit inclusion and exclusion criteria for MS patients and autoimmune diseases; outcomes were detailed accordingly, and all research involved individuals diagnosed with MS according to established MS diagnostic criteria. Funding sources differed with each study. Table 8 presents these findings.
Discussion
Neurodegeneration represents a fundamental feature of MS, characterized by axonal damage, myelin loss, and neuronal degeneration. MSC therapy has shown potential not only for modulating immune responses but also for offering neuroprotective benefits. This section examines how MSC transplantation affects CSF biomarkers related to neuroprotection and assesses their utility as indicators of treatment efficacy in MS. These biomarkers encompass both pro-inflammatory and anti-inflammatory markers. The reviewed studies highlight that MSCs promote the development of Tregs and inhibit pro-inflammatory Th17 cells, helping restore immune homeostasis. This systematic review concluded that MSC therapy is generally safe and well tolerated, and leads to improvements in disability levels and a reduction in lesion burden for a significant number of individuals with MS.
Impact of MSC Transplantation on CSF Neuroprotective Biomarkers
Neurofilament light chains (NF-L) and CXC motif chemokine ligand 13 (CXCL13) have been demonstrated to function as dependable biomarkers for both inflammatory processes and neurodegenerative changes in the context of MS. Elevated concentrations of NF-L have been consistently identified in the CSF of individuals diagnosed with MS, indicating that NF-L may serve as a significant biomarker for assessing disease activity, as well as the efficacy of various therapeutic interventions for MS [31]. One study showed that CSF concentrations of NF-L were significantly diminished six months after treatment with MSCs in patients diagnosed with progressive MS (p-value <0.05). CXCL13 concentrations were also lower; however, this reduction did not reach statistical significance. MSC transplantation may have a neuroprotective effect on MS patients, according to the study’s findings [20]. In contrast, another study found no changes in CSF-NfL levels after IT MSC injections, which contrasts with the previously mentioned study that found decreased NfL levels [21]. This contradiction requires larger-scale studies with a more extended follow-up to confirm these observations. Differences in CSF-NfL findings may be attributed to several factors, including variation in MSC source (e.g., autologous bone marrow vs. umbilical cord vs. MSC-NP), dose and frequency of administration, and the route of delivery (IT vs. IV). Additionally, the timing of post-treatment sampling and patient-specific disease characteristics (e.g., disease stage or baseline inflammatory activity) could influence biomarker dynamics and partially explain these inconsistencies. These considerations highlight the need for standardized protocols in future studies.
Furthermore, the study revealed elevated levels of matrix metalloproteinase-9 (MMP9) and reduced levels of chemokine ligand 2 (CCL2) in the CSF following treatment with intrathecal mesenchymal stem cell-neural progenitors (IT MSC-NPs) in cases of progressive multiple sclerosis (PMS), indicating possible neuroprotective properties and the modulation of neuroinflammatory responses. Elevated MMP9 post-MSC-NP treatment may target cells involved in CNS repair and regeneration, while decreased CCL2 levels indicate a reduction in neuroinflammation, possibly influencing disease progression [21]. Remarkably, after fetal neural stem cell transplantation (SCT), there was also an increase in CSF MMP9 levels in MS patients [32]. The regenerative response linked to IT cell therapy is further implied to be biomarked by MMP9 [21]. Furthermore, the increase of MMP9 and the decrease of CCL2 in the CSF following MSC-NP therapy act as biochemical indicators of the treatment, suggesting its potential efficacy in patients with MS.
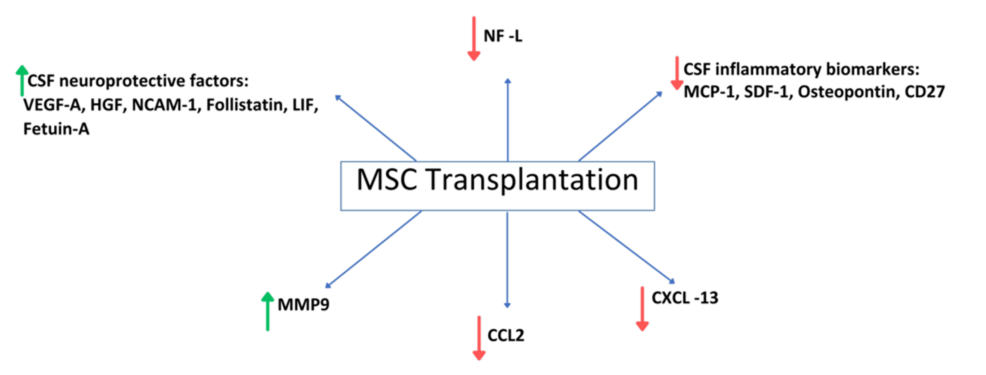
According to another recent study, treatment with autologous MSC-NTF-secreting cells in PMS led to a noteworthy increase in CSF neuroprotective factors like vascular endothelial growth factor A (VEGF-A), hepatocyte growth factor (HGF), neural cell adhesion molecule 1 (NCAM-1), follistatin, leukemia inhibitory factor (LIF), and fetuin-A, and a reduction in inflammatory biomarkers such as monocyte chemoattractant protein-1 (MCP-1), stromal cell-derived factor 1 (SDF-1), osteopontin, and CD27 [27]. These findings suggest a potential therapeutic benefit that warrants further investigation through randomized studies to explore the utility of CSF neurodegenerative biomarkers as outcome measures in PMS treatment evaluation, as the limited sample size may influence the assessment of these biomarkers [27].
Neurodegenerative and inflammatory biomarkers have provided essential biological insights into PMS, with CSF biomarkers indicating inflammation in the CNS [33,34]. In addition to these preliminary results, examining immunosoluble factors in the CSF of individuals with PMS revealed two categories of immune mediators. One group was characterized by pro-inflammatory activities, including IFN-γ (interferon gamma), MCP-1, TNF-α (tumor necrosis factor alpha), MIP-1α (macrophage inflammatory protein-1 alpha), MIP-1β (macrophage inflammatory protein-1 beta), IL-8 (interleukin-8), and IP-10 (interferon gamma-induced protein 10), while the other comprised anti-inflammatory factors such as IL-9, IL-15, IL-1ra, and VEGF [26]. These findings provide significant insights into the immune mechanisms implicated in PMS, underscoring the need for further investigation of these biomarkers in relation to disease progression, diagnostic accuracy, and predictive responses to treatment. Moreover, significant changes in the biomarkers present in CSF were noted following treatment with MSCs, supporting the clinical findings reported in the literature [21]. Figure 2 illustrates these findings.
Immunomodulatory Mechanisms of MSCs Therapy in MS
MS is an immune-mediated inflammatory condition characterized by dysregulated, pro-inflammatory CD4+ T cells in the CNS, leading to non-traumatic disabilities in young adults [35,36]. A key cellular marker for remission in MS is the increase in CD4+ T cells, which includes Tregs, that play a crucial role in reducing inflammation associated with the disease. A recent study demonstrated that administering UC-MSCs intrathecally to MS patients improved disability scales, lymphocyte counts, and various disease metrics, highlighting the potential of MSC therapy for MS treatment. The results indicated a notable rise in CD4+ T cells, particularly the Treg subset, at 12 months following treatment (p-value < 0.05). In contrast, natural killer (NK) cell levels further declined in these patients, indicating an immune-suppressive effect. This suggests that giving MS patients two doses of treatment may improve their immune responses [28]. Furthermore, larger multisite studies with similar or higher doses of MSCs are needed to validate the findings and optimize therapy protocols for MS treatment.
Moreover, an imbalance between Th17 cells and Tregs plays a significant role in the pathogenesis of MS [37-39]. The breakdown of peripheral immune tolerance triggers the activation of autoreactive CD4+ T cells within the lymph nodes, particularly Th1 and Th17 cells, which then evolve into highly aggressive effector cells, including both Th1 and Th17 phenotypes [35]. In addition, prior research has demonstrated that mitochondrial disorders of CD4+ T cells can alter their metabolic patterns in MS patients. This can result in a disruption of CD4+ T cell subset differentiation, which, in turn, can cause a Th17/Treg skew towards Th17 cells and intensify the inflammatory response in vivo [40]. An alternative viewpoint for investigating the mechanism of MSCs in MS therapy is offered by this pathway. It increases the therapeutic potential of stem cells and helps position MSC-based cell therapy as a cutting-edge approach that targets specific organelles [14].
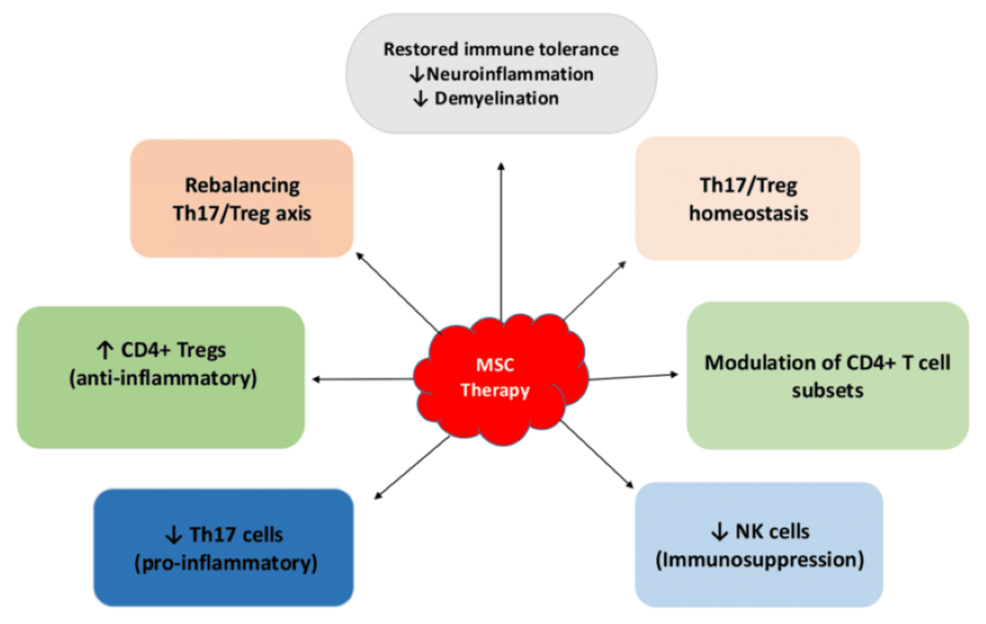
Specifically, MSCs inhibit the differentiation of Th17 and Th1 cells, while concurrently promoting the differentiation of Treg cells and influencing macrophage polarization to enhance the formation of anti-inflammatory M2 macrophages in preference to pro-inflammatory M1 macrophages [15,16]. Furthermore, MSC injection affects the differentiation of CD4+ T cells. This effect is evident in the induction of anergy and a reduction in Th17 cell populations, which facilitates the polarization of antigen-specific Treg cells. Such a mechanism aids in rectifying the imbalance within the Th17/Treg axis, consequently reducing the inflammatory response and demyelination, while promoting an overall state of immune tolerance [14]. Apart from the above, the study showed that MSC therapy regulates Th17/Treg homeostasis via extracellular vesicles, metabolic reprogramming, mitochondrial transfer, and autophagy. These pathways are essential for restoring immune self-stabilization and tolerance, thereby reducing neuroinflammation and demyelination linked to MS. Considering the significant relationship between cellular metabolism and immunoregulatory networks, compounds that facilitate mitochondrial translocation and metabolic reprogramming could represent valuable targets for MSCs in the regulation of immune homeostasis, as well as for identifying novel therapeutic avenues for MS via cellular therapy [14]. However, MSC therapy remains in an early investigational stage, with further clinical studies needed to validate its safety and therapeutic efficacy. The flowchart in Figure 3 summarizes the immunomodulatory mechanism of MSC therapy.
Safety, Efficacy, and Clinical Outcomes of MSC Therapy
Clinical trials indicate that SCT can lead to significant clinical recovery and enhanced quality of life for patients with MS, with few safety issues reported [41,42]. A recent study evaluated the effectiveness and safety of SCT for MS, incorporating data from nine RCTs with 422 participants. The results indicated that SCT significantly surpassed the control group in enhancing patients’ Expanded Disability Status Scale (EDSS) scores at the two-month interval (p-value = 0.03) and in decreasing the volume of MRI-T2-weighted lesions (p-value = 0.0002) [29]. The procedure was largely safe and well-tolerated, with no reported fatalities or major serious adverse events, aside from infusion site reactions following MSC therapy during the follow-up period. Patients receiving MSC therapy did report localized adverse events at the infusion site. According to these findings, SCT may help people with MS reduce their brain lesion volume and lessen their disability, while maintaining a generally acceptable safety profile. However, further research is required to confirm these findings and evaluate their long-term implications [29].
Similarly, one study evaluated 18 RCTs to investigate whether MSC transplantation is safe and effective in treating a range of autoimmune diseases, including MS [30]. MSCs may have a positive influence on several autoimmune conditions, according to these findings, potentially decreasing disease activity and improving clinical symptoms. Importantly, no significant adverse events associated with MSC transplantation were reported, indicating the generally safe nature of this treatment. However, the results concerning MS were less definitive; while some studies indicated symptom improvements, inconsistencies in dosage and administration techniques led to controversial overall outcomes, underlining the necessity for further research [30]. Additionally, this research offers promising insights into the use of MSCs for treating autoimmune diseases, highlighting potential benefits and safety, while emphasizing the need for further RCTs to refine or confirm these conclusions.
The results of a similar study assessed the changes in EDSS scores from baseline to follow-up and revealed that around 40.4% (95% CI: 30.6-50.2) of MS patients experienced improvement following MSC therapy, while 32.8% (95% CI: 25.5-40.1) remained stable, maintaining their condition, and 18.1% (95% CI: 12.0-24.2) of patients saw a decline in their health. Although no significant complications were reported, some minor adverse effects, such as headaches and fever, were observed. These findings suggest that a significant proportion of MS patients experienced benefits from MSC therapy, underscoring its potential as a viable treatment option [6]. Furthermore, the lack of significant adverse events suggests this therapeutic strategy is safe for MS patients. This study offers important insights into the effectiveness and safety of MSC therapy in managing MS, presenting a comprehensive understanding of its benefits for individuals with this condition [6]. Nevertheless, more studies, technological advancements, MSC dose optimization, and larger clinical trials are crucial for a comprehensive assessment of the long-term effectiveness and safety profiles of MSC therapy in MS patients.
Limitations
This systematic review thoroughly followed PRISMA 2020 guidelines. The study encompasses a combination of recent RCTs, non-RCTs, narrative reviews, systematic reviews, and high-quality meta-analyses. We comprehensively searched the literature through databases, including studies published in the last five years (from 2020 to 2025), to find more recent research and create precise results. We also included grey literature and other databases. We could disregard past research that might have relevant findings.
Despite the encouraging findings, which revealed statistically significant results emphasizing the safety benefits of MSCs as a neuroprotective and immunomodulatory potential therapy in MS patients, several limitations constrain the interpretation and generalizability of the current evidence. First, sample size limitations were a significant concern in many of the included studies. Second, the heterogeneity of MSC preparations and administration protocols complicates direct comparisons of studies. Various studies have used different MSC sources (bone marrow, umbilical cord, or autologous MSC-NTF), delivery routes (IT vs. IV), and dosing schedules, which may account for the conflicting outcomes. Third, the short follow-up durations in many trials limit the understanding of the long-term effects and sustainability of clinical and biomarker improvements. Additionally, the lack of double-blinded, placebo-controlled designs in several trials introduces a risk of bias, particularly in subjective outcome measures, such as the EDSS.
In addition, the absence of a formal assessment of publication bias was primarily due to the heterogeneous nature of the included studies, which varied in design, size, and outcome reporting. Nevertheless, this represents a potential source of bias, as studies with negative results may be underrepresented in the published literature. Future systematic reviews with larger sample sizes and more homogeneous datasets should incorporate publication bias analyses to better evaluate the robustness of reported effects. Moreover, variations in follow-up duration and study heterogeneity may result in inconsistent conclusions. The review’s limitations underscore the need for future research to undertake larger, standardized, multi-center trials with extended follow-up and thorough safety evaluations.
Conclusions
In conclusion, the studies included in this review show that exploring MSC therapy for MS has revealed a significant array of encouraging findings related to its neuroprotective and immunomodulatory effects. A comprehensive systematic review of the existing literature highlights that the transplantation of MSCs has a major impact on CSF biomarkers related to neuroprotection, including NF-L and CXCL13. These biomarkers are vital markers of inflammation and neuronal health, indicating that MSC therapy may be important for preserving the integrity and functionality of the brain. Additionally, MSCs promote immune balance by modulating T cell populations, which is vital in a condition characterized by immune-mediated damage. Initial findings regarding the safety and effectiveness of MSC therapy are promising, indicating improvements in disability and reductions in lesion burden. This growing body of research holds substantial promise for developing innovative treatment strategies tailored for individuals affected by MS. By addressing the neurodegenerative features and the immune dysregulation associated with the disease, MSC therapy could enhance intervention effectiveness and improve the quality of life for affected individuals. Future suggestions for this study include conducting additional research, prioritizing the standardization of MSC treatment protocols, and implementing larger, RCTs with longer follow-up durations. Such studies are crucial for validating the therapeutic potential of MSCs in MS, thereby providing a clearer understanding of their long-term effects and mechanisms of action.
References
- Walton C, King R, Rechtman L, et al.: Rising prevalence of multiple sclerosis worldwide: insights from the Atlas of MS, third edition. Mult Scler. 2020, 26:1816-21. 10.1177/1352458520970841
- van Langelaar J, Rijvers L, Smolders J, van Luijn MM: B and T cells driving multiple sclerosis: identity, mechanisms and potential triggers. Front Immunol. 2020, 11:760. 10.3389/fimmu.2020.00760
- Bar-Or A, Li R: Cellular immunology of relapsing multiple sclerosis: interactions, checks, and balances. Lancet Neurol. 2021, 20:470-83. 10.1016/S1474-4422(21)00063-6
- Balasa R, Barcutean L, Balasa A, Motataianu A, Roman-Filip C, Manu D: The action of TH17 cells on blood brain barrier in multiple sclerosis and experimental autoimmune encephalomyelitis. Hum Immunol. 2020, 81:237-43. 10.1016/j.humimm.2020.02.009
- Gugliandolo A, Bramanti P, Mazzon E: Mesenchymal stem cells in multiple sclerosis: recent evidence from pre-clinical to clinical studies. Int J Mol Sci. 2020, 21:8662. 10.3390/ijms21228662
- Islam MA, Alam SS, Kundu S, Ahmed S, Sultana S, Patar A, Hossan T: Mesenchymal stem cell therapy in multiple sclerosis: a systematic review and meta-analysis. J Clin Med. 2023, 12:6311. 10.3390/jcm12196311
- Dumitrescu L, Papathanasiou A, Coclitu C, Constantinescu CS, Popescu BO, Tanasescu R: Beta interferons as immunotherapy in multiple sclerosis: a new outlook on a classic drug during the COVID-19 pandemic. QJM. 2021, 114:691-7. 10.1093/qjmed/hcaa348
- Melnikov M, Sharanova S, Sviridova A, et al.: The influence of glatiramer acetate on Th17-immune response in multiple sclerosis. PLoS One. 2020, 15:e0240305. 10.1371/journal.pone.0240305
- Chun J, Giovannoni G, Hunter SF: Sphingosine 1-phosphate receptor modulator therapy for multiple sclerosis: differential downstream receptor signalling and clinical profile effects. Drugs. 2021, 81:207-31. 10.1007/s40265-020-01431-8
- McGinley MP, Goldschmidt CH, Rae-Grant AD: Diagnosis and treatment of multiple sclerosis: a review. JAMA. 2021, 325:765-79. 10.1001/jama.2020.26858
- Stamatellos VP, Papazisis G: Safety and monitoring of the treatment with disease-modifying therapies (DMTS) for multiple sclerosis (MS). Curr Rev Clin Exp Pharmacol. 2023, 18:39-50. 10.2174/2772432817666220412110720
- Wang Y, Fang J, Liu B, Shao C, Shi Y: Reciprocal regulation of mesenchymal stem cells and immune responses. Cell Stem Cell. 2022, 29:1515-30. 10.1016/j.stem.2022.10.001
- Chen B, Chen Z, He M, Zhang L, Yang L, Wei L: Recent advances in the role of mesenchymal stem cells as modulators in autoinflammatory diseases. Front Immunol. 2024, 15:1525380. 10.3389/fimmu.2024.1525380
- Hu H, Li H, Li R, Liu P, Liu H: Re-establishing immune tolerance in multiple sclerosis: focusing on novel mechanisms of mesenchymal stem cell regulation of Th17/Treg balance. J Transl Med. 2024, 22:663. 10.1186/s12967-024-05450-x
- Song N, Scholtemeijer M, Shah K: Mesenchymal stem cell immunomodulation: mechanisms and therapeutic potential. Trends Pharmacol Sci. 2020, 41:653-64. 10.1016/j.tips.2020.06.009
- Jiang W, Xu J: Immune modulation by mesenchymal stem cells. Cell Prolif. 2020, 53:e12712. 10.1111/cpr.12712
- Zhou T, Li HY, Liao C, Lin W, Lin S: Clinical efficacy and safety of mesenchymal stem cells for systemic lupus erythematosus. Stem Cells Int. 2020, 2020:6518508. 10.1155/2020/6518508
- Margiana R, Markov A, Zekiy AO, et al.: Clinical application of mesenchymal stem cell in regenerative medicine: a narrative review. Stem Cell Res Ther. 2022, 13:366. 10.1186/s13287-022-03054-0
- Smith JA, Nicaise AM, Ionescu RB, Hamel R, Peruzzotti-Jametti L, Pluchino S: Stem cell therapies for progressive multiple sclerosis. Front Cell Dev Biol. 2021, 9:696434. 10.3389/fcell.2021.696434
- Petrou P, Kassis I, Ginzberg A, Hallimi M, Karussis D: Effects of mesenchymal stem cell transplantation on cerebrospinal fluid biomarkers in progressive multiple sclerosis. Stem Cells Transl Med. 2022, 11:55-8. 10.1093/stcltm/szab017
- Harris VK, Stark J, Williams A, et al.: Efficacy of intrathecal mesenchymal stem cell-neural progenitor therapy in progressive MS: results from a phase II, randomized, placebo-controlled clinical trial. Stem Cell Res Ther. 2024, 15:151. 10.1186/s13287-024-03765-6
- Page MJ, McKenzie JE, Bossuyt PM, et al.: The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Syst Rev. 2021, 10:89. 10.1186/s13643-021-01626-4
- Higgins JP, Altman DG, Gøtzsche PC, et al.: The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ. 2011, 343:d5928. 10.1136/bmj.d5928
- Tufanaru C, Munn Z, Aromataris E, Campbell J, Hopp L: JBI Manual for evidence synthesis. JBI Reviewer’s Manual. Aromataris E, Munn Z (ed): JBI, 2020. 10.46658/JBIMES-20-04
- Shea BJ, Reeves BC, Wells G, et al.: AMSTAR 2: a critical appraisal tool for systematic reviews that include randomised or non-randomised studies of healthcare interventions, or both. BMJ. 2017, 358:j4008. 10.1136/bmj.j4008
- Baethge C, Goldbeck-Wood S, Mertens S: SANRA-a scale for the quality assessment of narrative review articles. Res Integr Peer Rev. 2019, 4:5. 10.1186/s41073-019-0064-8
- Cohen JA, Lublin FD, Lock C, et al.: Evaluation of neurotrophic factor secreting mesenchymal stem cells in progressive multiple sclerosis. Mult Scler. 2023, 29:92-106. 10.1177/13524585221122156
- Jamali F, Aldughmi M, Atiani S, et al.: Human umbilical cord-derived mesenchymal stem cells in the treatment of multiple sclerosis patients: phase I/II dose-finding clinical study. Cell Transplant. 2024, 33:3045. 10.1177/09636897241233045
- Nawar AA, Farid AM, Wally R, et al.: Efficacy and safety of stem cell transplantation for multiple sclerosis: a systematic review and meta-analysis of randomized controlled trials. Sci Rep. 2024, 14:12545. 10.1038/s41598-024-62726-4
- Zeng L, Yu G, Yang K, Xiang W, Li J, Chen H: Efficacy and safety of mesenchymal stem cell transplantation in the treatment of autoimmune diseases (rheumatoid arthritis, systemic lupus erythematosus, inflammatory bowel disease, multiple sclerosis, and ankylosing spondylitis): a systematic review and meta-analysis of randomized controlled trial. Stem Cells Int. 2022, 2022:9463314. 10.1155/2022/9463314
- Williams T, Zetterberg H, Chataway J: Neurofilaments in progressive multiple sclerosis: a systematic review. J Neurol. 2021, 268:3212-22. 10.1007/s00415-020-09917-x
- Genchi A, Brambilla E, Sangalli F, et al.: Neural stem cell transplantation in patients with progressive multiple sclerosis: an open-label, phase 1 study. Nat Med. 2023, 29:75-85. 10.1038/s41591-022-02097-3
- Donninelli G, Studer V, Brambilla L, et al.: Immune soluble factors in the cerebrospinal fluid of progressive multiple sclerosis patients segregate into two groups. Front Immunol. 2021, 12:633167. 10.3389/fimmu.2021.633167
- Kapoor R, Smith KE, Allegretta M, et al.: Serum neurofilament light as a biomarker in progressive multiple sclerosis. Neurology. 2020, 95:436-44. 10.1212/WNL.0000000000010346
- Li R, Li H, Yang X, Hu H, Liu P, Liu H: Crosstalk between dendritic cells and regulatory T cells: protective effect and therapeutic potential in multiple sclerosis. Front Immunol. 2022, 13:970508. 10.3389/fimmu.2022.970508
- Moser T, Akgün K, Proschmann U, Sellner J, Ziemssen T: The role of TH17 cells in multiple sclerosis: therapeutic implications. Autoimmun Rev. 2020, 19:102647. 10.1016/j.autrev.2020.102647
- Karimi E, Azari H, Tahmasebi A, et al.: LncRNA-miRNA network analysis across the Th17 cell line reveals biomarker potency of lncRNA NEAT1 and KCNQ1OT1 in multiple sclerosis. J Cell Mol Med. 2022, 26:2351-62. 10.1111/jcmm.17256
- Shi C, Zhang J, Wang H, et al.: Trojan horse nanocapsule enabled in situ modulation of the phenotypic conversion of Th17 cells to Treg cells for the treatment of multiple sclerosis in mice. Adv Mater. 2023, 35:e2210262. 10.1002/adma.202210262
- Fujiwara M, Raheja R, Garo LP, et al.: microRNA-92a promotes CNS autoimmunity by modulating the regulatory and inflammatory T cell balance. J Clin Invest. 2022, 132:e155693. 10.1172/JCI155693
- Greeck VB, Williams SK, Haas J, Wildemann B, Fairless R: Alterations in lymphocytic metabolism-an emerging hallmark of MS pathophysiology?. Int J Mol Sci. 2023, 24:2094. 10.3390/ijms24032094
- Markov A, Thangavelu L, Aravindhan S, et al.: Mesenchymal stem/stromal cells as a valuable source for the treatment of immune-mediated disorders. Stem Cell Res Ther. 2021, 12:192. 10.1186/s13287-021-02265-1
- Oliveira AG, Gonçalves M, Ferreira H, Neves N: Growing evidence supporting the use of mesenchymal stem cell therapies in multiple sclerosis: a systematic review. Mult Scler Relat Disord. 2020, 38:101860. 10.1016/j.msard.2019.101860